Sequelae of Infection of Dental Pulp
Periapical infection with Streptococci & Staphylococci
Majority of streptococci produce hyaluronidase, an enzyme that dissolves hyaluronic acid which is a universal intercellular cementing substance. It helps in the spread of infection. Usually staphylococci are good producers of hyaluronidase, so there is no spread of infection and the infection becomes localised in the form of abscess in case of staph infection.
Streptococci are also producers of fibrinolysin that dissolves fibrin. Along With Hyaluronidase, it causes the spread of infection into tissue spaces resulting in cellulitis.
A dental abscess may develop directly from in a necrotic pulp or often it originates in an area of chronic infection e. g. periapical granuloma.
Ludwig Angina
Ludwig angina is the advanced stage of cellulitis. It usually begins in the submaxillary space and later involves the sublingual and submental spaces. The main source of infection is second and third molars. Most cases show mixed infection and streptococci are invariably present.
In Ludwig Angina, if 2nd premolar and 1st molar are involved then sublingual space is involved primarily as their apices lie above the mylohyoid attachment level. On the contrary, if 2nd and third molars are involved, submaxillary space primarily gets involved as their apices lie below mylohyoid attachment level.
Acute Osteomyelitis
In acute osteomyelitis little or no radiographic features are seen for at least one or two weeks. Later, diffuse lytic changes in the bone begins to appear. individual trabeculae becomes hazy and indistinct. Radiolucent area begins to appear. In earlier stages of chronic osteomyelitis mottled appearance is seen in radiographs. In established cases of osteomyelitis moth eaten appearance is seen because of enlargement of medullary spaces and widening of Volkmann’s canal.
The most common organism cultured from the osteomyelitis lesions include staphylococcus aureus and staphylococcus Albus.
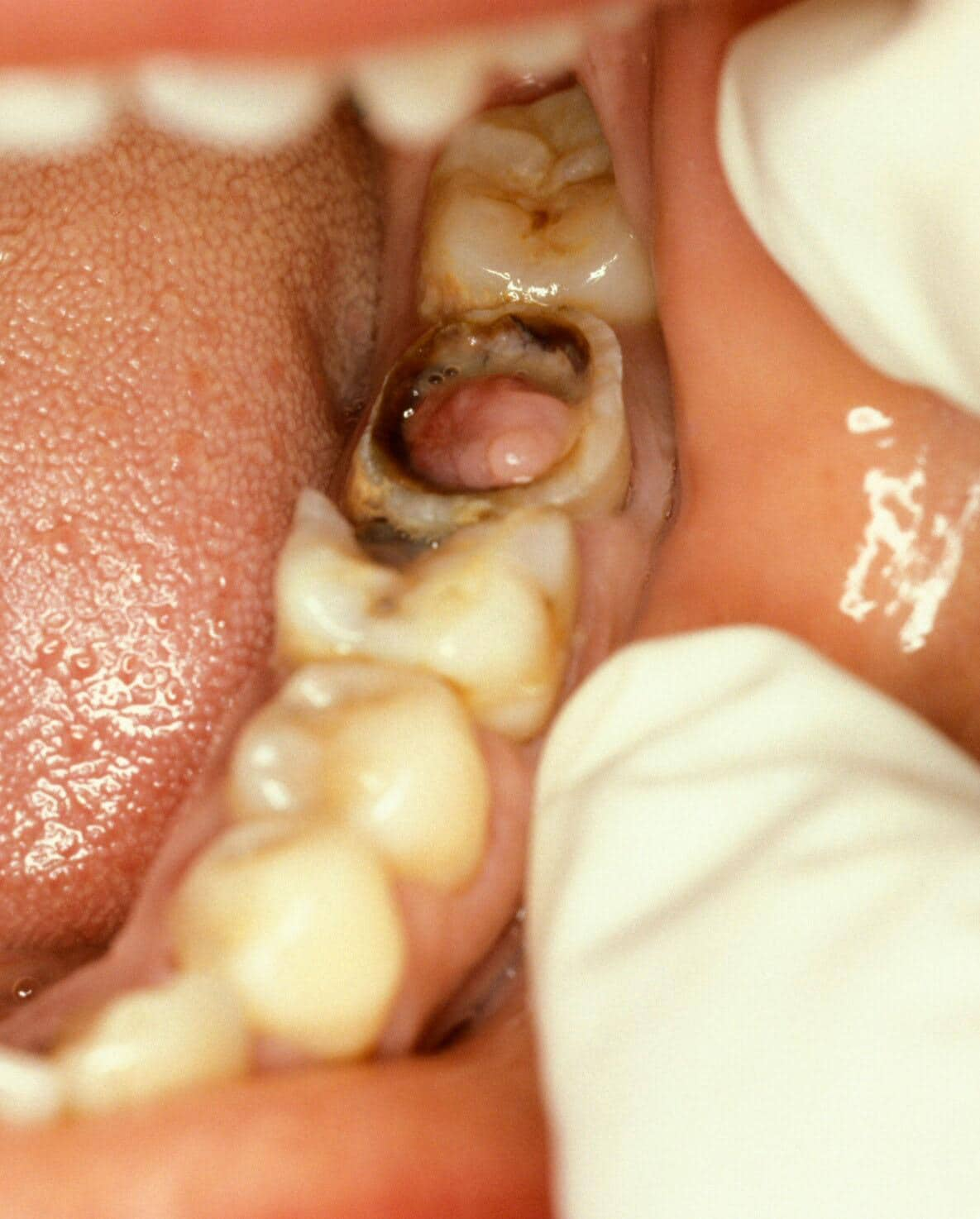
Chronic Hyperplastic Pulpitis
A pulp polyp appears as a dusky red or pinkish soft nodule protruding from the pulp to fill a carious cavity. It is painless but may be tender and bleed on probing. It should be distinguished from proliferating gingival tissue extending over the edge of the cavity by tracing its attachment.
When a pulp polyp starts developing, the pulp converts itself and is replaced by granulation tissue. The polyp surface is ultimately epithelialized and covered by a layer of well-formed stratified squamous epithelium. The stratified squamous epithelium gives safety to the granulation tissue and helps inflammation to subside. It also helps the granulation tissue to mature into fibrous tissue. The same level of pulpal proliferation can often be seen in teeth with fully formed roots but is most common in children. As in open pulpits, this is because open apices provide a better blood supply and prevent the pulp from dying as a result of pulpal oedema.
Periapical Granuloma/Chronic Apical Periodontitis
The cells of periapical granuloma which are predominantly lymphocytes increase by division at the periphery.
The cells in the centre are separated from their source of nutrition; hence degenerate and liquify. This results in an epithelium lined cavity filled with fluid known as periapical cyst.
Condensing Osteitis
In condensing osteitis the periodontal ligament space is widened and this is an important feature in distinguishing from cementoblastoma.
Ref:
1. Ref: Medscape-https://reference.medscape.com/