Odontogenic Keratocyst
Odontogenic keratocyst (OKC) is a parakeratin lined cyst like lesion within bone.
OKCs mostly occur in the 2nd and 3rd decades of life; although can occur over a wide age range with male predilection. Odontogenic keratocyst comprises of 4 to 12 percent of all odontogenic cysts. Ninety percent of odontogenic keratocysts are solitary. Multiple cysts are found in Nevoid Basal Cell Carcinoma Syndrome / Gorlin Syndrome[1].
The most commonly involved body part in mandible, 65-85%; mostly posterior mandible. Normally, they are associated with third molars but may be present without associating with third molars; rarely occur in soft tissues.
They are considered to arise from dental lamina.
Clinical Features
Odontogenic keratocysts are often asymptomatic. They are incidentally discovered on radiographs. They can cause symptomatic swelling. They can cause parasthesia of lip and teeth. Symptoms of pain and drainage are found if secondarily infected. They can cause local bone and soft tissue destruction, but usually spare teeth and roots.
 |
| Swelling observed at the right buccal mucosa (dotted area) posterior to the orifice of Stensen’s duct-arrow head [3]. |
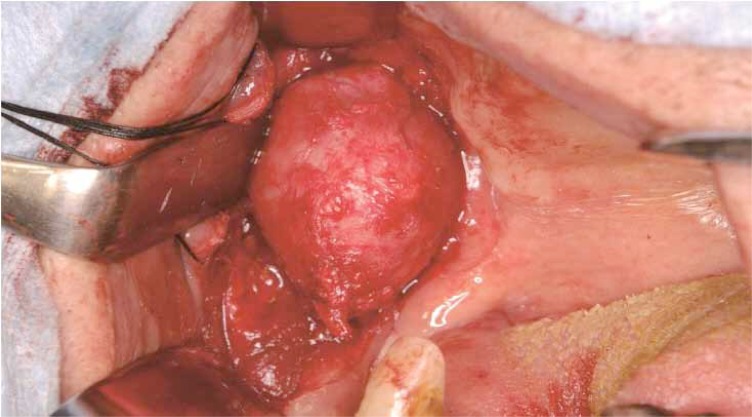 |
| Odontogenic keratocyst-exposed anterior to the masseter muscle. |
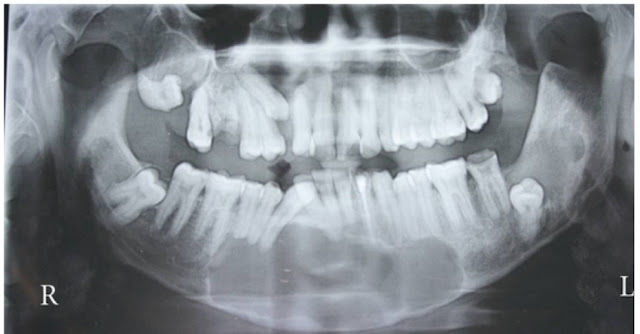
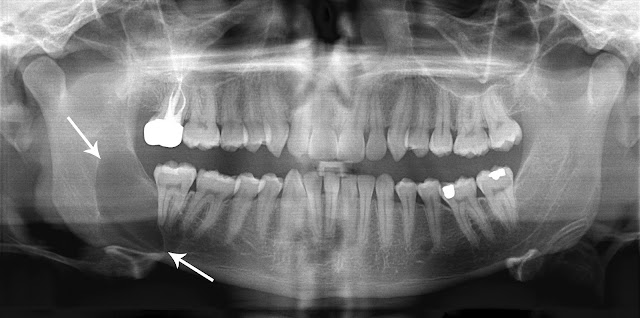
Radiographic features
Mostly, they are seen as small unilocular radiolucent lesions with variable sclerotic margins. Larger lesions are often seen multilocular with variable scalloped margins. Therefore, They may resemble radicular cyst, dentigerous cyst, lateral periodontal cyst, and ameloblastoma.
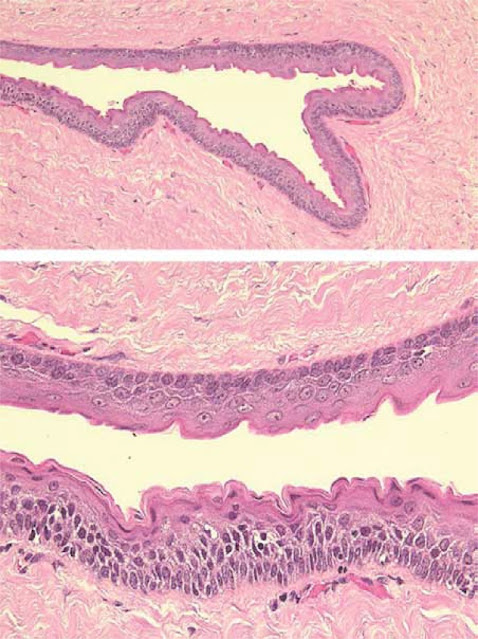
Histology
Differential Diagnosis
- Ameloblastoma
- Dentigerous cyst
- Peri-apical cyst
- Lateral periodontal cyst
Prognosis
Recurrence rates of OKC are from 20% to 56% with enucleation alone. Resection have been reported to have no recurrences, but it may be considered excessive for a benign cyst.Treatment
- Decompression.
- Enucleation with possible curettage.
- Chemical curettage with Carnoy’s solution.
- Marsupialization.
- Resection.
Case Studies
Ref:
- Morrison A. Odontogenic keratocyst. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/mandiblemaxillakeratocyst.html. Accessed September 11th, 2022.
- https://en.wikipedia.org/wiki/File:Classic_keratocystic_odontogenic_tumour.jpg
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3837368/figure/F1/
- https://www.pathologyoutlines.com/caseofweek/case503.htm
- K. M. Veena, Rekha Rao, H. Jagadishchandra, Prasanna Kumar Rao, "Odontogenic Keratocyst Looks Can Be Deceptive, Causing Endodontic Misdiagnosis", Case Reports in Pathology, vol. 2011, Article ID 159501, 3 pages, 2011. https://doi.org/10.1155/2011/159501