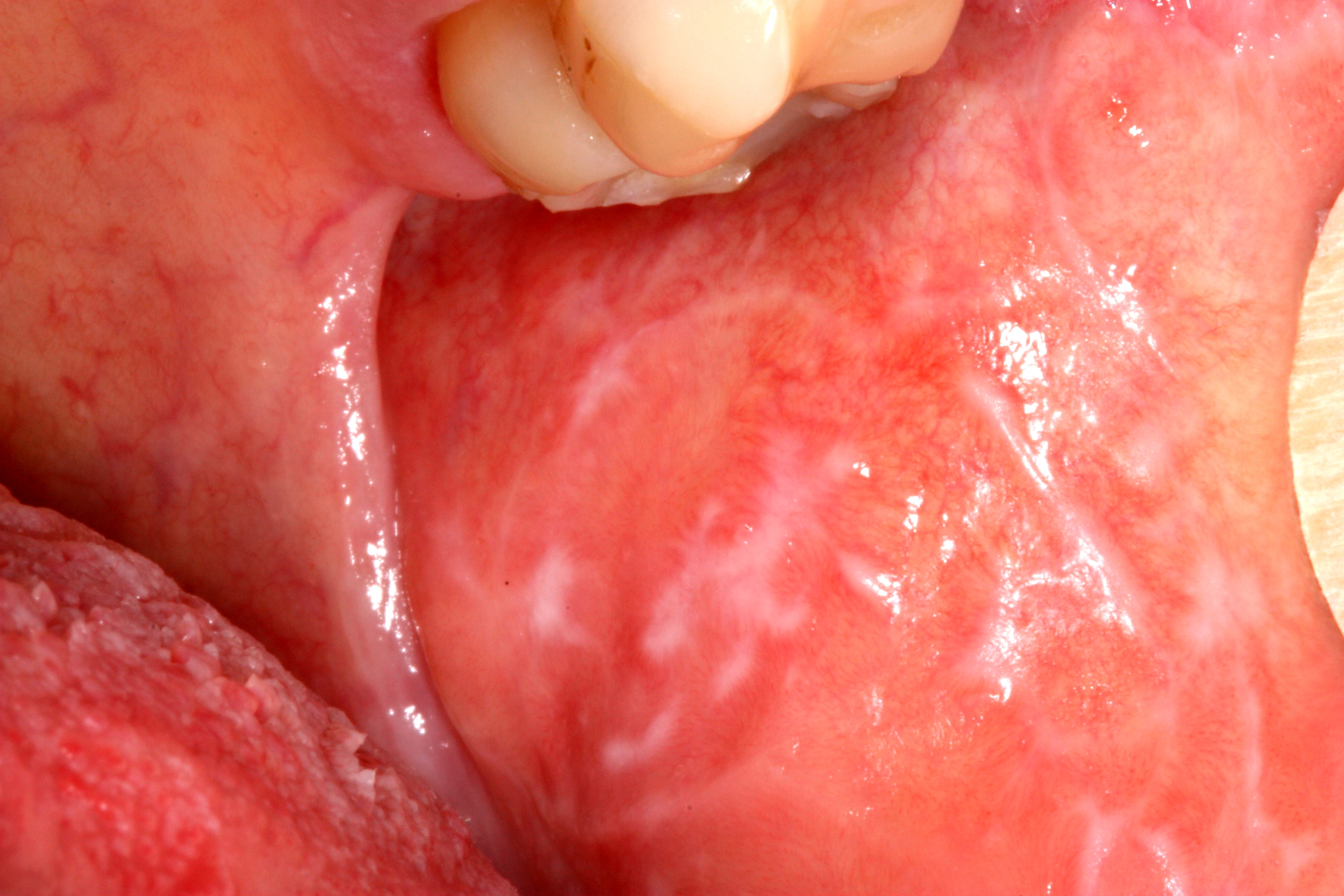
Oral mucosal lesions are common. They can be due to physiological changes or a local disease. They may also be an oral manifestation of a skin condition, an adverse drug reaction or systemic disease, for example, gastrointestinal disease. To manage an oral mucosal disease successfully one requires an accurate diagnosis.
Now the question arises, how will we get an accurate diagnosis?
The correct answer is, by a thorough assessment of oral mucosa for a lesion.
Assessment for an oral mucosal lesion involves taking a full patient history. This includes a medication history too. Next we need to perform a thorough extraoral and intraoral examination and use diagnostic investigations where appropriate. One should have a high index of suspicion for oral cancer.
To recognise oral cancer one should be familiar with the risk factors for oral cancer. You can see the “Oral Cancer” topic to know about risk factors for oral cancer. You should also thoroughly know the red flag features of oral cancer. If any 'red flag' features are present or the diagnosis is not clear or the patient has not responded to initial treatment, early referral to an appropriate specialist is required. An oral medicine specialist is the most appropriate specialist to diagnose and manage oral mucosal disease, but may not be accessible. Therefore, an oral surgeon, dermatologist or otorhinolaryngologist are other options.
Failure to respond to initial treatment, an unclear diagnosis or the presence of any suspicious features could indicate malignancy and warrant early referral.
‘Red flag’ features of oral mucosal disease
oral ulcers that have lasted for more than 2 weeks
orals ulcers that recur
nontraumatic oral ulcers in children
pigmented lesions on the oral mucosa
red, white or mixed red and white lesions on the oral mucosa of unknown origin or with features of potentially malignant disease, such as: induration, ulceration with rolled margins, fixation to underlying tissues, lesions in high-risk sites (eg lateral tongue, floor of mouth)
facial or oral paraesthesia
persistent oral mucosal discomfort with no obvious cause
lumps or swellings, including lymphadenopathy
swelling, pain or blockage of a salivary gland, suggestive of salivary gland disease
suspected allergy or adverse reaction to dental materials for example oral lichenoid lesion, dry mouth that is not adequately relieved with artificial salivary products and nonpharmacological methods and dry mouth caused by systemic disease
suspected oral manifestations of systemic disease, for example, syphilis, Behçet syndrome, HIV, inflammatory bowel disease, lichen planus, pemphigoid
lesions occurring in immunocompromised patients, for example, patients with neutropenia or HIV infection
Some oral mucosal diseases are associated with significant morbidity and mortality, particularly oral potentially malignant disorders and oral cancer. Oral potentially malignant disorders include:
- oral leukoplakia
- oral erythroplakia
- chronic hyperplastic candidiasis
- actinic cheilitis
- oral lichen planus
- oral submucous fibrosis
- discoid lupus erythematosus
- dyskeratosis congenita
- epidermolysis bullosa
Oral potentially malignant disorders can become malignant at the site of the lesion, but also predict an increased risk of cancer at other sites in the mouth, even in clinically normal appearing oral mucosa.
The following conditions can be managed in general practice, provided there are no 'red flag' features present that would warrant referral:
recurrent aphthous ulcerative disease
traumatic oral ulcers
oral candidiasis
angular cheilitis
oral mucocutaneous herpes simplex virus
dry mouth
oral mucositis
amalgam tattoo
geographic tongue
hairy tongue.
There are physiological causes of oral mucosal discolorations, for example, Fordyce spots which are ectopic sebaceous glands and leukoedema, that do not require active management.
Ref:
Therapeutic guidelines (oral & dental) 2019