Normally there is one opening of the parotid gland which is located in buccal vestibule opposite the upper 2nd molar tooth.
Parotid fistula is a patent tract connecting a parotid gland or duct to the exterior apart from the parotid duct opening.
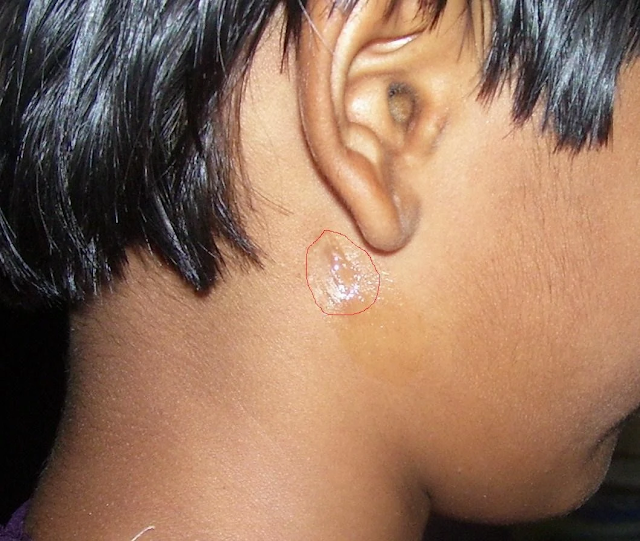 |
| Photo 1. Pre-operative picture of parotid fistula with leakage of serous fluid from the fistulous tract and scarring of surrounding area (red circle) [1] |
Parotid
fistula may be of two types
1. Glandular:
It arises directly from gland. It shows minimal discharge during rest or eating.
2. Ductal: It
arises from duct. It shows profuse discharge during eating.
Parotid fistula may be extra oral or intraoral.
Extraoral fistulas are seen in the preauricular region or near the angle of mandible (see photo 1 and 2).
 |
| Photo 2. showing discharge of serous fluid from the right cheek in the angle of mandible region [2] |
Causes
1. After superficial parotidectomy.
2. After drainage of parotid abscess.
3. After biopsy or Trauma.
4. Post surgical
Clinical Features
1.
Discharging fistula in the parotid region of the face, and discharge is more during eating.
2. Tenderness and induration.
3. Trismus if it gets infected
Diagnosis
1.
Sialography to find out the origin of the fistula whether from the parotid gland or duct or ductules.
2. Fistulogram or CT fistulogram.
3. Culture of discharge if infection is
suspected
4. MRI to assess soft tissues
involvement
Treatment
Ø Surgical stripping of the fistula
tract
Ø Anticholinergics in post-operative
period- Hyoscine bromide (Probanthine) reduce discharge
Ø Immediate post surgical fistulas can
close spontaneously in such cases
Ø Newman Seabrock's operation: used for
removal of anomalous arotid fistula
Ø If there is stenosis at the orifice
of the Stenson's duct, papillotomy at the orifice may help.
Ø Total conservative parotidectomy is
done in failed cases conserving the facial nerve
Ref: